
The severely ill heart patient
Objectives
- To further develop and test the "intelligent bed" for home use among severely ill heart patients in their own homes.
- To prevent re-admissions of severely ill heart patients.
- To increase the quality of life and security for severely ill heart patients in their own homes using the intelligent bed.
- To improve the working environment for home care staff, so as to release time for restructured work routines.
- To develop a business case for the use of the intelligent bed in home care.
Target group
Patients with chronic heart disease are divided into 4 groups, the fourth group being those patients with the most severe symptoms. Patients in group 4 often suffer from one or more derivative diseases and can have severe symptoms (surplus water in the body, fatigue, irregular heartbeat, etc.), that can cause them to be partially bedridden at times. The goal is that 6-8 patients can test the intelligent bed for two months at a time.
Scenario
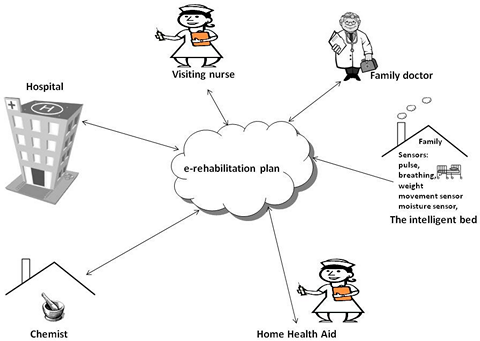
Marie Nielsen is 72 years old and has had a heart condition for many years. Marie’s condition is so severe that she has been hospitalized many times because of water in the lungs and irregular heartbeat. Marie has had a hospital bed at home because her own bed cannot be elevated sufficiently at the head and leg ends. Marie gets rapid swelling of the legs, perspires a lot and has a tendency to shortness of breath because of her weak heart. She cannot walk very far and must rest most of the day in bed. Three to four times per day, she is visited by a home health aid who helps her with personal hygiene, and a nurse comes twice a day to administer medication and to observe Marie, as she can quickly develop symptoms of pulmonary edema. Marie has a daughter who works long hours and lives 40 km away, so the daughter cannot always come when Marie calls. Living alone at home, this situation causes Marie to feel uncomfortable at times. Marie was offered the opportunity to test the intelligent bed with the following functions: safety, weight, oxygen, breathing, moisture and motion sensors and voice function. Data from the functions is transmitted to an e-rehabilitation plan and can be monitored by the home care service, by the nurse, by Marie herself and by her daughter. Depending on Marie's condition, the functions can be set to measure and transmit data whenever Marie's own physician deems it appropriate. Marie is happy about the voice function, as she can now contact the nurse without calling for "emergency assistance" and she can contact her daughter if need be. Both Marie and her daughter feel comfortable with this new technology. If Marie starts to develop any symptoms of pulmonary edema, it can be discovered quickly, as the nurse has time to come and examine Marie and summon a doctor if necessary. Marie can quickly obtain diuretic medication and avoid admission to hospital because symptoms have been identified early.